-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 7 issue 3
Computerized tomography scan in acute appendicitis with eventual negative appendectomy
Ming Li Chia*, Kwan Justin, Hui Terrence Chi Hong, Shelat Vishal G
Chia et al. J Clin Transl Res 2021; 7(3):5
Published online: May 27, 2021
Abstract
Background: Acute appendicitis (AA) is traditionally considered a clinical diagnosis and negative appendectomy (NA) rates vary across healthcare systems. Computed tomography (CT) scans have been shown to aid in the reduction of NA rates. Our study aimed to determine the preoperative imaging characteristics in patients undergoing appendectomy with eventual normal histology.
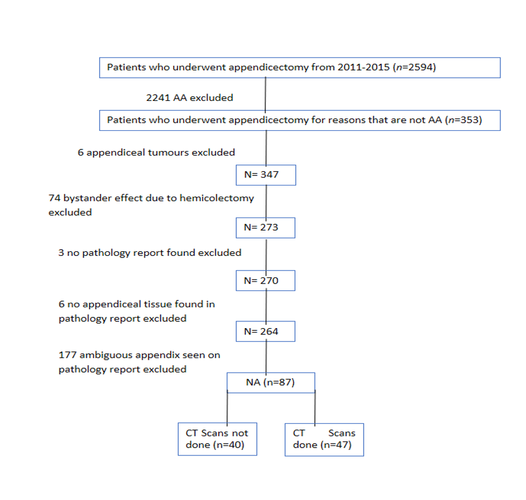
Methods: An audit of all patients with a discharge diagnosis of AA was conducted from January 2011 to December 2015. Histology reports of all patients who underwent appendectomies were reviewed, and medical records of patients with NA were included in the study. To study the impact of CT scan reporting in NA patients, CT scan images of patients with NA were reviewed retrospectively by two blinded radiologists.
Results: 2603 patients underwent appendectomy for suspected AA, and NA rate was 3.34% (n=87). The mean age of patients with NA was 30.3 (14.8-69.8) years with no gender difference (51.7 % male). 66 (75.9%) patients had laparoscopic appendectomy with a 3.5% open conversion rate. CT scans were done in 47 patients. Preoperative CT scan report was more likely to report dilated appendix (n=26(55.3%) vs. n=7(14.9%), p=0.0001). Postoperative blinded radiology review was more like to report other pathology (n=27(57.4%) vs. n=2(4.3%), p=0.0001) and normal appendix (n=26(55.3%) vs. n=5(10.6%), p=0.0001).
Conclusions: The NA rate is low. There needs to be standardized reporting for imaging features of prominent / dilated appendix.
Relevance for patients: Appendectomy must be avoided in patients with a normal CT scan and when another pathological diagnosis is established. Liberal imaging policy assists to reduce negative appendectomy rates. Imaging features of prominent or dilated appendix can be subjective and international collaboration is needed to define thresholds for imaging diagnosis of acute appendicitis.
DOI: http://dx.doi.org/10.18053/jctres.07.202103.005
Author affiliation
1. Lee Kong Chian School of Medicine, Singapore
2. Department of Radiology, Tan Tock Seng Hospital, Singapore
3. Department of General Surgery, Tan Tock Seng Hospital, Singapore
*Corresponding author
Ming Li Chia
Lee Kong Chian School of Medicine, 11 Mandalay Road, Singapore 308232
Tel: +65 93202101
Email: mingli.chia@mohh.com.sg
Handling editor:
Michal Heger
Department of Pharmaceutics, Utrecht University, the Netherlands
Department of Pharmaceutics, Jiaxing University Medical College, Zhejiang, China

