-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 8 Issue 5
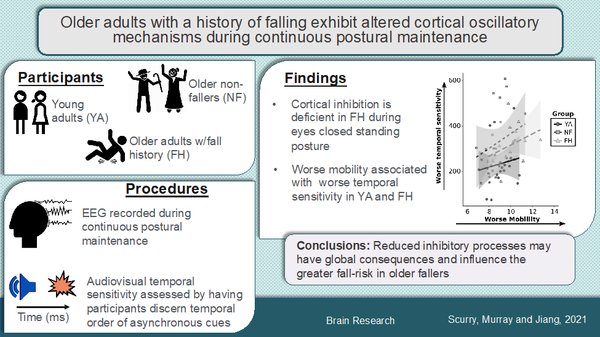
Older adults with a history of falling exhibit altered cortical oscillatory mechanisms during continuous postural maintenance
Alexandra N. Scurry, Brian Szekely, Nicholas G. Murray, Fang Jiang*
Scurry et al. J Clin Transl Res 2022; 8(5):2
Published online: September 7, 2022
Abstract
Background and aim: The significant risk of falling in older adults 65 years or older presents a substantial problem for these individuals, their caretakers, and the healthcare system at large. As the proportion of older adults in the United States is only expected to grow over the next few decades, a better understanding of physiological and cortical changes that make an older adult more susceptible to a fall is crucial. Prior studies have displayed differences in postural dynamics and stability in older adults with a fall history (FH) and those that have never fallen (NF), suggesting surplus alterations that occur in some older adults (i.e. FH group) in addition to the natural aging process.
Methods: The present study measured postural dynamics while FH, NF and young adult (YA) groups performed continuous postural maintenance. In addition, EEG activity was recorded while participants performed upright postural stance to examine any group differences in cortical areas involved in postural control.
Results: As expected, older participants (FH and NF) exhibited worse postural stability, as evidenced by increased excursion, compared to the YA group. Further, while NF and YA show increased alpha activity in occipital areas during the most demanding postural task (eyes closed), FH group did not show any differences in occipital alpha power between postural tasks.
Conclusions: As alpha activity reflects suppression of bottom-up processing and thus diversion of cognitive resources toward postural centers during more demanding postural maintenance, deficits in this regulatory function in the FH group is a possible impaired cortical mechanism putting these individuals at greater fall risk.
Relevance for patients: Impaired inhibitory function in older adults may impact postural control and increase their risk of falling. Interventions that aim at addressing cortical processing deficits may improve postural stability and facilitate independent living in this population.
DOI: http://dx.doi.org/10.18053/jctres.08.202205.002
Author affiliation
1. Department of Psychology, University of Nevada, Reno, NV 89557 USA
2. School of Public Health, University of Nevada, Reno, NV 89557 USA
*Corresponding author
Fang Jiang
Department of Psychology, University of Nevada, Reno, NV 89557 USA
Email: fangj@unr.edu
Handling editor:
Michal Heger
Department of Pharmaceutics, Utrecht University, the Netherlands
Department of Pharmaceutics, Jiaxing University Medical College, Zhejiang, China

