-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 9 Issue 1
Etiological spectrum of isolated ileo-cecal ulcers in patients with gastrointestinal symptoms
Mayank Bhushan Pateria, Anurag Kumar Tiwari, Vinod Kumar, Dawesh P Yadav, Sunit Kumar Shukla, Ashutosh Gupta, Gurvachan Singh, Vinod Kumar Dixit*
Pateria et al. J Clin Transl Res 2023; 9(1):3
Published online: December 14, 2022
Abstract
Background: Isolated ileo-cecal region ulcers may represent underlying Crohn’s disease, intestinal tuberculosis, bacterial infections (including typhoid), amoebiasis, eosinophilic enteritis, drug-induced sequelae, or neoplasm. Overlapping morphological and microscopic characteristics of many of these diseases make it challenging to unequivocally confirm a diagnosis.
Aims: To investigate the etiology and clinical outcomes of isolated ileo-cecal ulcers discovered during an ileocolonoscopy in patients with gastrointestinal symptoms.
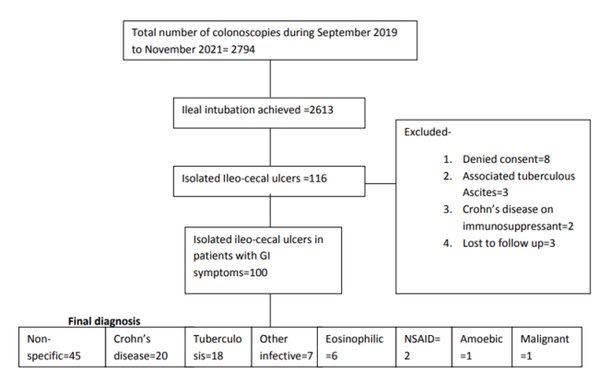
Methods: Patients with isolated ileo-cecal ulcers and symptoms within the age range of 10 to 80 years were included (N = 100). Patients not giving consent (assent in case of a minor), with a prior diagnosis of tuberculosis or inflammatory bowel disease, with incomplete colonoscopy and associated colonic lesions other than ileo-cecal region were excluded from the study. Demographics, clinical information, and relevant biochemical and serological tests were recorded. During the colonoscopy, multiple biopsies were taken from the ileo-cecal ulcers for histopathological examination. Repeat ileocolonoscopy was performed as needed in consenting patients.
Results: The mean age and mean duration of symptoms were 36.0 ± 15.6 years and 18.8 ± 21.6 months, respectively. The majority of the patients presented with abdominal pain (59%), followed by diarrhea (47%), weight loss (20%), gastrointestinal bleeding (15%), and fever (11%). A history of taking non-steroidal anti-inflammatory drugs was present in only 5% of the patients. Mean hemoglobin, C-reactive protein, and albumin levels were 11.6 ± 2.8 g/dl, 6.9 ± 9.5 mg/l, and 3.7 ± 0.8 g/dl, respectively. Based on clinical, colonoscopic, and histopathological findings, initial treatment was symptomatic/antibiotics in 55%, anti-tubercular treatment in 21%, 5-aminosalicylic acid/steroids for Crohn’s disease in 13%, oral budesonide in 10% of patients, and one patient was referred for management of malignancy. Final diagnoses after 8-24 weeks of follow-up were non-specific ileitis/colitis (45%), Crohn’s disease (20%), intestinal tuberculosis (18%), infective (7%), eosinophilic ileitis/colitis (6%), non-steroidal anti-inflammatory drug-induced (2%), and amoebic and malignant in 1% of patients each.
Conclusions: The majority of patients with ileo-cecal ulcers have specific etiologies. Non-specific ulcers at the ileo-cecal region can be managed symptomatically; however close follow-up is necessary as sometimes the ulcers may harbor an underlying specific disease.
Relevance for patients: Isolated ileo-cecal ulcers are common findings during colonoscopy in both symptomatic and asymptomatic patients. The majority of these ulcers harbor underlying significant diseases that can cause morbidity and mortality if left undiagnosed and untreated. Reaching a specific diagnosis in such cases is not straightforward, and patients are often subjected to repeat examinations.
DOI: http://dx.doi.org/10.18053/jctres.09.202301.003
Author affiliation
Department of Gastroenterology, Institute of Medical Sciences, Banaras Hindu University, Varanasi – 221005, India
*Corresponding author
Vinod Kumar Dixit
Department of Gastroenterology, Institute of Medical Sciences, Banaras Hindu University, Varanasi – 221005, India.
Tel: +91 941 520 2449
E-mail: drvkdixit@gmail.com
Handling editor:
Michal Heger
Department of Pharmaceutics, Utrecht University, the Netherlands
Department of Chemistry, Utrecht University, Utrecht, the Netherlands
Department of Pathology, Erasmus Medical Center, the Netherlands
Department of Pharmaceutics, Jiaxing University Medical College, Zhejiang, China

