-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 1 Issue 1
Layer-by-layer heparinization of decellularized liver matrices to reduce thrombogenicity of recellularized liver grafts
Bote G. Bruinsma, Yeonhee Kim, Tim A. Berendsen, Sinan Ozer, Martin L. Yarmush, Basak E. Uygun
Bruinsma et al., J Clin Transl Res, 2015; 1(1): 48-56
Published online: 19 July, 2015
Abstract
Background: Tissue engineered liver grafts may offer a viable alternative to orthotopic liver transplantation
and help overcome the donor organ shortage. Decellularized liver matrices (DLM) have a preserved
vasculature and sustain hepatocellular function in culture, but graft survival after transplantation remains
limited due to thrombogenicity of the matrix.
Aim: To evaluate the effect of heparin immobilization on DLM thrombogenicity.
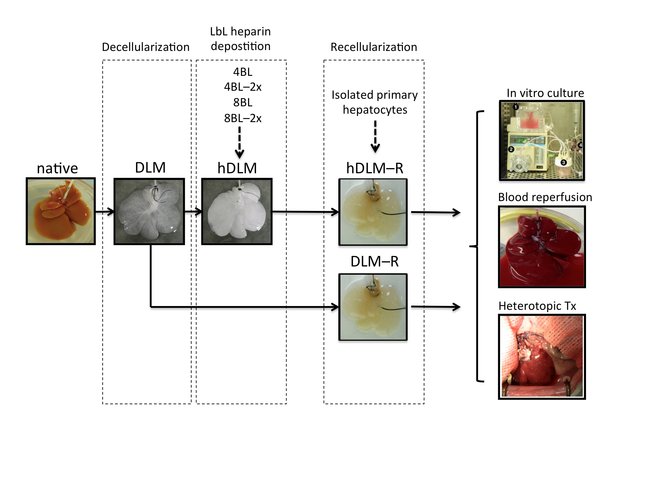
Methods: Heparin was immobilized on DLMs by means of layer-by-layer deposition. Grafts with 4 or 8
bilayers and 2 or 4 g/L of heparin were recellularized with primary rat hepatocytes and maintained in culture
for 5 days. Hemocompatibility of the graft was assessed by ex vivo diluted whole-blood perfusion and
heterotopic transplantation.
Results: Heparin was deposited throughout the matrix and the heparin content in the graft was higher with
increasing number of bilayers and concentration of heparin. Recellularization and in vitro albumin and urea
production were unaffected by heparinization. Resistance to blood flow during ex vivo perfusion was lower
with increased heparinization and, macroscopically, no clots were visible in grafts with 8 bilayers. Following
transplantation, flow through the graft was limited in all groups. Histological evidence of thrombosis
was lower in heparinized DLMs, but transplantation of DLM grafts was not improved.
Conclusions: Layer-by-layer deposition of heparin on a DLM is an effective method of immobilizing heparin
throughout the graft and does not impede recellularization or hepatocellular function in vitro. Thrombogenicity
during ex vivo blood perfusion was reduced in heparinized grafts and optimal with 8 bilayers, but
transplantation remained unsuccessful with this method.
Relevance for patients: Tissue engineered liver grafts may offer a viable solution to dramatic shortages in
donor organs
Doi: http://dx.doi.org/10.18053/jctres.201501.004
Author affiliation
1 Center for Engineering in Medicine, Department of Surgery, Massachusetts General Hospital, Harvard Medical School, and the Shriners Hospitals for Children, Boston, Massachusettes, United States
2 Department of Surgery (Surgical Laboratory), Academic Medical Center, University of Amsterdam, Amsterdam, the Netherlands
3 Department of Biomedical Engineering, Rutgers University, Piscataway, New Jersey, United States
*Corresponding author: Basak E Uygun
51 Blossom Street, Boston, MA 02114, United States
Tel: +1 617 371 4879
Fax: +1 617 573 9471
Email: buygun@mgh.harvard.edu
Handling editor:
Rowan van Golen
Department of Experimental Surgery, Academic Medical Center, University of Amsterdam, Amsterdam, the Netherlands

